You have used the cream. The rash disappeared. You felt relieved.
Then, two weeks later — it is back. Maybe on the same spot. Maybe somewhere else. Maybe even worse than before.
This is one of the most frustrating complaints we hear at our Lucknow clinic.
Nearly every week, someone walks into our Chowk clinic and tells me, “Ma’am, this infection has come back for the fourth time.” or “I have used so many creams. Why does this rash not go away forever?”
Here is the truth that most people never learn:
Fungal infections do not keep coming back because they are “strong.” They keep coming back because something in your treatment or environment is wrong.
In this guide, we will explain exactly why your fungus returns, the hidden mistakes you might be making, and most importantly — how to stop it for good.
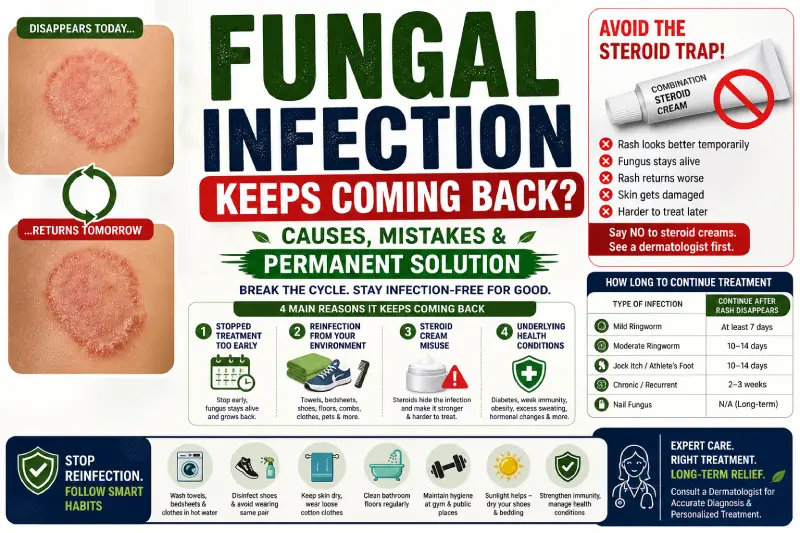
Why Fungal Infections Recur
There are four main reasons why your fungal infection keeps returning.
Let me walk you through each one.
Reason 1: You Stopped Treatment Too Early
This is the number one reason for recurrence.
Most antifungal creams need to be applied for 2 to 4 weeks depending on the severity of your infection.
Here is what happens when you stop early:
| What You Do | What Actually Happens |
| Rash disappears at day 7 | You think you are cured |
| You stop applying cream | You feel happy and relieved |
| Fungus is still alive underneath | You cannot see it because rash is gone |
| Within 10-14 days | Fungus grows back, rash returns |
The rule: Continue your treatment for at least 7 days AFTER your rash completely disappears — not when it starts looking better.
For chronic or widespread infections, your dermatologist may ask you to continue for 2-3 weeks after visible clearance.
Reason 2: You Are Getting Reinfected From Your Own Environment
Even if you complete your full treatment, you can catch the same fungus again from things you touch every day.
Fungal spores can survive on surfaces for weeks or even months.
Common sources of reinfection in your home:
- Towels — Fungi love damp towels. If you share towels with family members, you can pass the infection back and forth.
- Bedsheets and pillowcases — Your skin touches these for 6-8 hours every night.
- Shoes — Athlete’s foot fungus lives inside shoes. If you wore the same shoes during your infection, the fungus is still there.
- Bathroom floors — Walking barefoot on damp bathroom tiles spreads fungus.
- Combs and hair brushes — Scalp fungus can live on combs.
- Clothing — Tight, sweaty clothes worn during infection need proper washing.
- Gym equipment and yoga mats — Public places are common sources of reinfection.
- Pets — Dogs and cats can carry ringworm without showing symptoms.
Reason 3: You Fell Into the Steroid Cream Trap
This is dangerous and very common.
Many patients walk into a chemist shop with an itchy rash and walk out with a cream containing steroids — often without even knowing it.
Creams like Betnovate, Diprovate, and Quadriderm contain potent steroids.
Here is why steroid creams are disastrous for fungal infections:
| Day | What You See | What Is Really Happening |
| Day 1-2 | Rash looks better | Steroid reduces swelling and itching temporarily |
| Day 5-7 | Rash disappears completely | You believe you are cured |
| Day 10-14 | Rash comes back | Fungus was never killed — only suppressed |
| Week 3 | Rash is larger and angrier | Fungus is now resistant to standard treatment |
| Month 2 | Skin looks thin, stretch marks appear | Steroid has permanently damaged your skin |
The worst part: Once you use steroids on a fungal infection, the fungus changes how it looks. Dermatologists call this “tinea incognito” — fungal infection disguised by steroids. It becomes harder to diagnose and harder to treat.
Advice: Never use any cream on a rash without knowing its ingredients. If a chemist recommends a “combination cream” — say no. See a dermatologist first.
Reason 4: You Have an Underlying Condition
Sometimes, recurrent fungal infections are a sign of something else going on inside your body.
Conditions that make you prone to repeated fungal infections:
- Diabetes — High blood sugar feeds fungi. Uncontrolled diabetes leads to frequent infections.
- Weak immune system — Due to medications, illness, or age.
- Obesity — Skin folds trap moisture, creating perfect fungal breeding grounds.
- Excessive sweating (hyperhidrosis) — Constant moisture on skin.
- Hormonal changes — Pregnancy, birth control pills, or thyroid issues.
If you have more than 3-4 fungal infections in a single year, your dermatologist may recommend tests to rule out underlying conditions.
How Long Should You Continue Treatment AFTER the Rash Disappears?
This is the most important question — and most people get it wrong.
| Type of Infection | Minimum Treatment Duration | Continue After Rash Disappears |
| Mild ringworm (small area) | 2 weeks | At least 7 days |
| Moderate ringworm (multiple areas) | 3-4 weeks | 10-14 days |
| Jock itch or athlete’s foot | 4 weeks | 10-14 days |
| Chronic or recurrent infection | 6-8 weeks | 2-3 weeks |
| Nail fungus | 6-12 months | N/A (different protocol) |
The golden rule: When you think you are done — continue for one more week.
Hidden Sources of Reinfection in Your Home
Let me give you a practical checklist.
After you complete your treatment, do these things — or your infection will return.
Immediate Actions (Within 24 Hours of Finishing Treatment)
- Wash all towels in hot water (60°C or above). Use an antifungal laundry sanitizer if available.
- Wash all bedsheets and pillowcases — same hot water method.
- Wash all clothes worn during the infection period, especially undergarments and socks.
- Disinfect your shoes — Spray inside with antifungal spray. Leave them in sunlight for a day. Do not wear the same shoes consecutively.
- Replace your bath loofah or scrubber — Throw away the old one.
- Clean bathroom floors with bleach or antifungal cleaner.
- Wash combs and hair brushes with hot soapy water or antifungal shampoo.
Weekly Habits to Prevent Recurrence
- Change your towel every 2-3 days (not once a week).
- Change bedsheets once weekly.
- Do not share towels, combs, or shoes with family members.
- Wear flip-flops in gyms, locker rooms, and hotel bathrooms.
Preventive Lifestyle Changes
Once you have broken the cycle of recurrence, these habits will keep fungus away permanently.
Daily Habits
- Dry your skin folds properly after bathing — Between toes, under breasts, groin area, armpits. Use a separate dry towel for these areas if needed.
- Use antifungal powder in high-risk areas during monsoon and summer months. Apply only on completely dry skin.
- Change out of sweaty clothes immediately — Do not let sweat dry on your body. Carry an extra set of clothes when commuting.
- Wear breathable fabrics — Cotton, bamboo, or moisture-wicking materials. Avoid synthetic, tight clothing in humid weather.
- Wear loose-fitting undergarments — Tight underwear traps moisture in groin area.
Weekly Habits
- Clean your sports footwear every week using an antifungal spray. If possible, wash them thoroughly.
- Give your shoes a full day to dry out before putting them back on your feet. Keep two or more pairs and switch between them.
- Your bath mats and bathroom rugs need hot water washing once every week.
When Stronger Medication Is Needed
Sometimes, topical creams are not enough.
Signs you may need oral antifungal medication:
- Your infection covers a large area of your body (more than 15-20% of skin surface)
- You have already tried 2-3 different topical creams without success
- Your infection keeps returning despite completing full treatment courses
- You have nail fungus (tablets are usually required)
- You have a weakened immune system or diabetes
- The infection is causing significant discomfort or affecting your daily life
Oral antifungals include:
- Terbinafine tablets
- Fluconazole tablets
- Itraconazole capsules
These are prescription-only medications. Your dermatologist will decide which one is right for you based on the type and severity of your infection. Some require liver function tests before and during treatment.
Complete Prevention Checklist
Use this checklist to make sure you are doing everything right.
| Category | Action | Done |
| Treatment | Completed full course (not stopped when rash disappeared) | ☐ |
| Treatment | Continued cream for 7+ days after rash vanished | ☐ |
| Laundry | Washed all towels in hot water | ☐ |
| Laundry | Washed all bedsheets in hot water | ☐ |
| Laundry | Washed all clothes from infection period | ☐ |
| Shoes | Disinfected all shoes with antifungal spray | ☐ |
| Shoes | Stopped wearing same shoes daily | ☐ |
| Bathroom | Cleaned bathroom floors with bleach | ☐ |
| Bathroom | Replaced bath loofah / scrubber | ☐ |
| Personal | Washed combs and brushes | ☐ |
| Personal | Stopped sharing towels with family | ☐ |
| Habits | Drying skin folds properly after bath | ☐ |
| Habits | Using antifungal powder in monsoon | ☐ |
| Habits | Changing sweaty clothes immediately | ☐ |
| Habits | Wearing cotton/breathable fabrics | ☐ |
When to See a Dermatologist
Do not keep suffering in silence. See us if:
- You have had 3 or more fungal infections in the past year
- Your infection does not improve after 2 weeks of over-the-counter antifungal cream
- Your infection spreads despite treatment
- You are living with diabetes or your immunity is compromised due to medication or illness
- You have used steroid creams on your rash without knowing
- The infection is on your face, scalp, or nails
Treatment Options at Dr. Asma Skin Clinic
If you are tired of recurring fungal infections, we can help.
| Service | What We Offer |
| KOH test | Painless, 2-minute confirmation of fungal infection |
| Prescription topicals | Stronger than over-the-counter creams |
| Oral antifungals | For severe, widespread, or recurrent cases |
| Steroid damage reversal | Treatment for skin damaged by steroid creams |
| Recurrence prevention plan | Long-term strategy customized for you |
| Underlying cause testing | Diabetes, immunity, and other conditions |
Frequently Asked Questions
Q: How do I know if my fungal infection is cured permanently?
A: You need to be symptom-free for at least 2-4 weeks after stopping treatment. If no rash returns during this time, you are likely cured.
Q: Can I catch the same fungal infection from my pet?
A: Yes. Dogs and cats can carry ringworm. If your pet has bald patches or scaly skin, have them checked by a veterinarian.
Q: Why does my jock itch keep coming back every summer?
A: Humidity and sweat trigger jock itch. You may need to use antifungal powder preventively during summer months, even when you have no active infection.
Q: Is it safe to use antifungal powder every day?
A: Yes, for high-risk individuals. Apply only on dry skin and avoid open wounds.
Q: Can my partner keep reinfecting me?
A: Absolutely. Fungal infections can travel between partners — sometimes without either person showing obvious signs. The infection may keep bouncing between you. To break this loop, both of you need treatment at the same time.
Q: How long before I can wear my old shoes again?
A: After disinfecting them with antifungal spray, wait 24-48 hours. Better yet, buy new socks and wear them only with disinfected shoes.
About Dr. Asma Parveen
Dr. Asma Parveen is a board-certified dermatologist with 14+ years of experience treating patients in Lucknow. She specializes in diagnosing and treating recurrent fungal infections, steroid-damaged skin, and chronic skin conditions.
At Lucknow clinic, she offers:
- Accurate KOH testing for confirmation
- Prescription-strength oral and topical antifungals
- Long-term recurrence prevention plans
- Treatment for underlying conditions causing recurrences
Ready to Stop Your Fungal Infection for Good?
You do not have to live with infections that keep coming back. With the right treatment and prevention strategy, you can break the cycle permanently.
New patients: 10% off first consultation
Visit our Clinic:
Dr. Asma MD Skin Clinic – Chowk, Lucknow
Subhash Chandra Bose Complex, Mandi Crossing, Victoria Street, Chowk Lucknow – 226003
Dr. Asma Skin & Hair Clinic – Thakurganj, Lucknow
Near Ghante Wala Sweets, Daulatganj Thakurganj, Lucknow – 226003
Dr. Asma Skin Clinic – Barabanki
Mohalla Ayodhya Nagar, Naka, Satrikh, Barabanki – 225001
Call/WhatsApp to Book Your Appointment: +91-9335312242